- Diabetes, obesity and metabolism
- Glucocorticoid-Induced Hyperglycemia: A Neglected Problem
-
Jung-Hwan Cho, Sunghwan Suh
-
Endocrinol Metab. 2024;39(2):222-238. Published online March 27, 2024
-
DOI: https://doi.org/10.3803/EnM.2024.1951
-
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
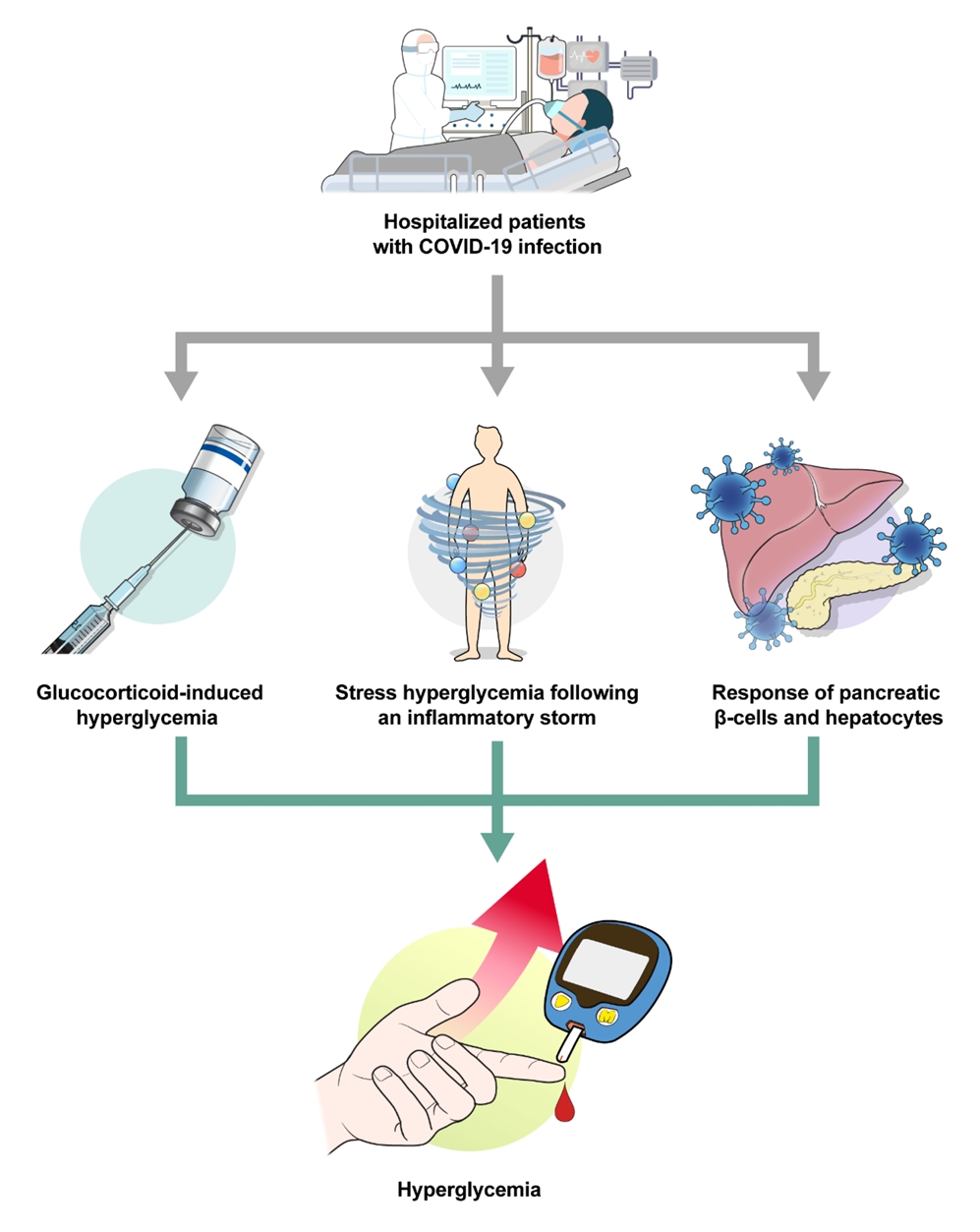
- Glucocorticoids provide a potent therapeutic response and are widely used to treat a variety of diseases, including coronavirus disease 2019 (COVID-19) infection. However, the issue of glucocorticoid-induced hyperglycemia (GIH), which is observed in over one-third of patients treated with glucocorticoids, is often neglected. To improve the clinical course and prognosis of diseases that necessitate glucocorticoid therapy, proper management of GIH is essential. The key pathophysiology of GIH includes systemic insulin resistance, which exacerbates hepatic steatosis and visceral obesity, as well as proteolysis and lipolysis of muscle and adipose tissue, coupled with β-cell dysfunction. For patients on glucocorticoid therapy, risk stratification should be conducted through a detailed baseline evaluation, and frequent glucose monitoring is recommended to detect the onset of GIH, particularly in high-risk individuals. Patients with confirmed GIH who require treatment should follow an insulin-centered regimen that varies depending on whether they are inpatients or outpatients, as well as the type and dosage of glucocorticoid used. The ideal strategy to maintain normoglycemia while preventing hypoglycemia is to combine basal-bolus insulin and correction doses with a continuous glucose monitoring system. This review focuses on the current understanding and latest evidence concerning GIH, incorporating insights gained from the COVID-19 pandemic.
- Diabetes, obesity and metabolism
- The Characteristics and Risk of Mortality in the Elderly Korean Population
-
Sunghwan Suh
-
Endocrinol Metab. 2023;38(5):522-524. Published online October 23, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.502
-
-
 PDF PDF PubReader PubReader  ePub ePub
- Diabetes, obesity and metabolism
- Greater Severity of Steatosis Is Associated with a Higher Risk of Incident Diabetes: A Retrospective Longitudinal Study
-
Ji Min Han, Jung Hwan Cho, Hye In Kim, Sunghwan Suh, Yu-Ji Lee, Jung Won Lee, Kwang Min Kim, Ji Cheol Bae
-
Endocrinol Metab. 2023;38(4):418-425. Published online July 12, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1729
-
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Fatty liver is associated with increased risk of developing type 2 diabetes. We aimed to evaluate whether the severity of hepatic steatosis is associated with incident diabetes.
Methods
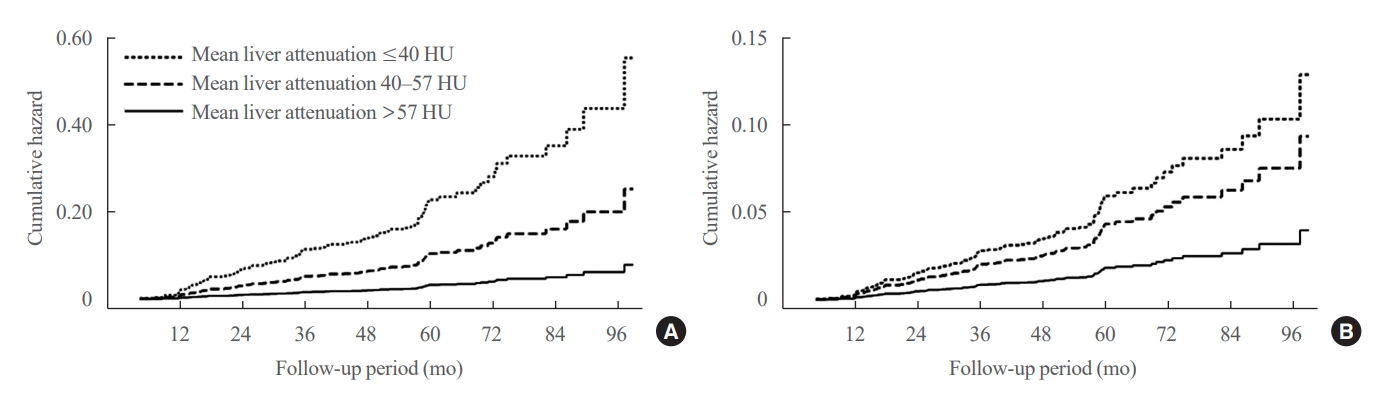
We conducted a longitudinal analysis using data from 1,798 participants who underwent a comprehensive health checkup and abdominal computed tomography (CT). We assessed the association between baseline liver attenuation value on non-contrast CT images and risk of incident diabetes. All the participants were categorized into three groups based on the baseline liver attenuation value on non-contrast CT images: without hepatic steatosis (>57 Hounsfield unit [HU]), mild hepatic steatosis (41–57 HU), and moderate to severe hepatic steatosis (≤40 HU).
Results
During a median follow-up period of 5 years, 6.0% of the study participants progressed to diabetes. The incidence of diabetes was 17.3% in the moderate to severe hepatic steatosis group, 9.0% in the mild steatosis group, and 2.9% in those without hepatic steatosis. In a multivariate adjustment model, as compared with participants without hepatic steatosis, those with moderate to severe steatosis had a hazard ratio (HR) of 3.24 (95% confidence interval [CI], 1.64 to 4.2) for the development of diabetes, and those in the mild steatosis group had a HR of 2.33 (95% CI, 1.42 to 3.80). One standard deviation decrease in mean CT attenuation values of the liver was associated with a 40% increase in the development of diabetes (multivariate adjusted HR, 1.40; 95% CI, 1.2 to 1.63).
Conclusion
We found a positive association between severity of hepatic steatosis and risk of incident diabetes. Greater severity of steatosis was associated with a higher risk of incident diabetes.
- Miscellaneous
- Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
-
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim, The Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2022;37(6):839-850. Published online December 26, 2022
-
DOI: https://doi.org/10.3803/EnM.2022.1627
-
-
3,571
View
-
321
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
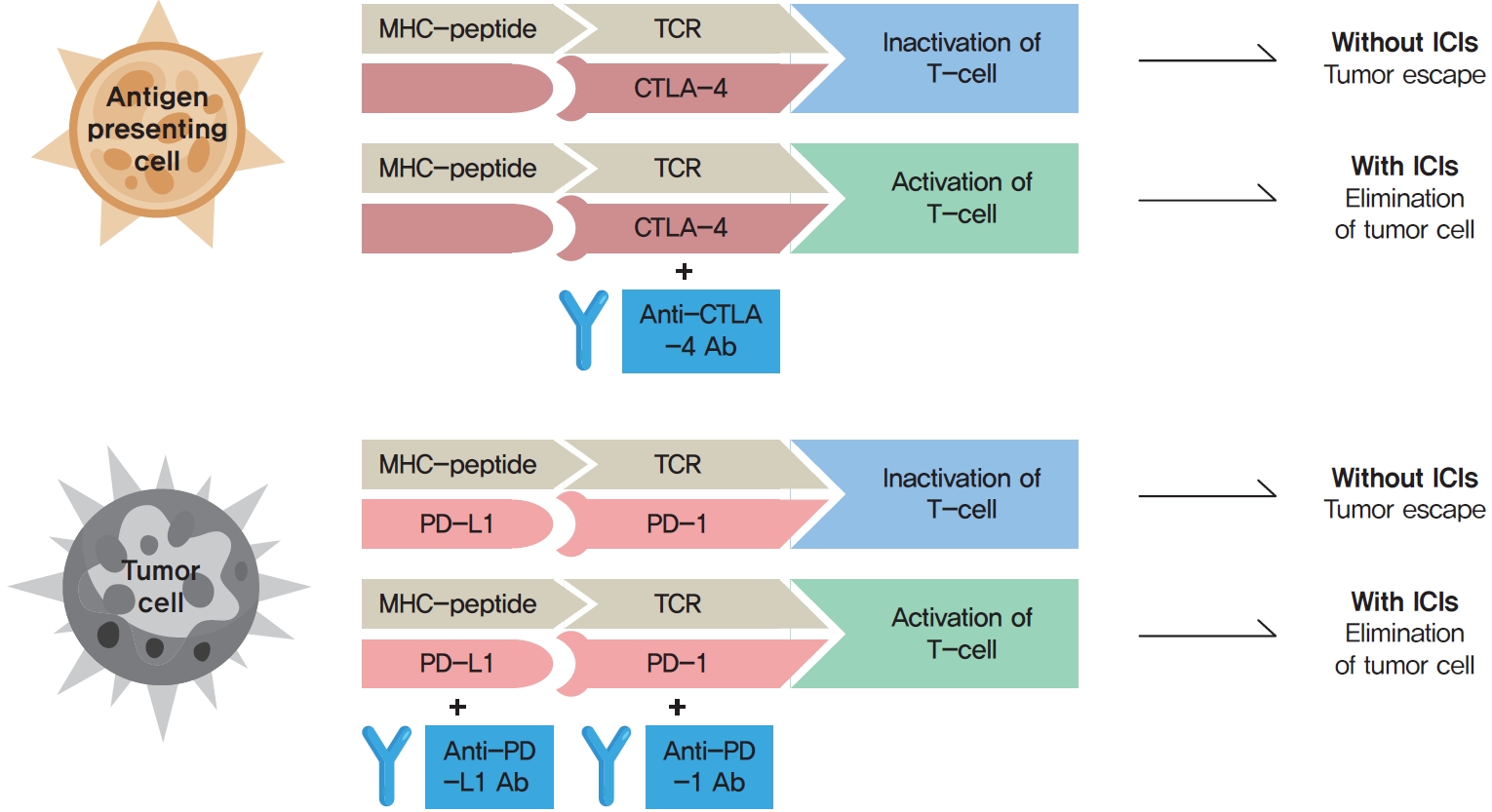
- Immune checkpoint inhibitors (ICIs) including an anti-cytotoxic T-lymphocyte-associated antigen 4 inhibitor, anti-programmed cell death protein 1 (PD-1) inhibitors, and anti-PD-ligand 1 inhibitors are representative therapeutics for various malignancies. In oncology, the application of ICIs is currently expanding to a wider range of malignancies due to their remarkable clinical outcomes. ICIs target immune checkpoints which suppress the activity of T-cells that are specific for tumor antigens, thereby allowing tumor cells to escape the immune response. However, immune checkpoints also play a crucial role in preventing autoimmune reactions. Therefore, ICIs targeting immune checkpoints can trigger various immune-related adverse events (irAEs), especially in endocrine organs. Considering the endocrine organs that are frequently involved, irAEs associated endocrinopathies are frequently life-threatening and have unfavorable clinical implications for patients. However, there are very limited data from large clinical trials that would inform the development of clinical guidelines for patients with irAEs associated endocrinopathies. Considering the current clinical situation, in which the scope and scale of the application of ICIs are increasing, position statements from clinical specialists play an essential role in providing the appropriate recommendations based on both medical evidence and clinical experience. As endocrinologists, we would like to present precautions and recommendations for the management of immune-related endocrine disorders, especially those involving the adrenal, thyroid, and pituitary glands caused by ICIs.
-
Citations
Citations to this article as recorded by  - Pembrolizumab plus lenvatinib for radically unresectable or metastatic renal cell carcinoma in the Japanese population
Ryo Fujiwara, Takeshi yuasa, kenichi kobayashi, tetsuya yoshida, susumu kageyama
Expert Review of Anticancer Therapy.2023; 23(5): 461. CrossRef - Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
Endocrinology and Metabolism.2023; 38(6): 750. CrossRef
- Miscellaneous
- COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
-
Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim, the Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2021;36(4):757-765. Published online August 17, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.404
-
-
10,437
View
-
419
Download
-
19
Web of Science
-
21
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Since the first outbreak of coronavirus disease 2019 (COVID-19), ongoing efforts have been made to discover an efficacious vaccine against COVID-19 to combat the pandemic. In most countries, both mRNA and DNA vaccines have been administered, and their side effects have also been reported. The clinical course of COVID-19 and the effects of vaccination against COVID-19 are both influenced by patients’ health status and involve a systemic physiological response. In view of the systemic function of endocrine hormones, endocrine disorders themselves and the therapeutics used to treat them can influence the outcomes of vaccination for COVID-19. However, there are very limited data to support the development of clinical guidelines for patients with specific medical backgrounds based on large clinical trials. In the current severe circumstances of the COVID-19 pandemic, position statements made by clinical specialists are essential to provide appropriate recommendations based on both medical evidence and clinical experiences. As endocrinologists, we would like to present the medical background of COVID-19 vaccination, as well as precautions to prevent the side effects of COVID-19 vaccination in patients with specific endocrine disorders, including adrenal insufficiency, diabetes mellitus, osteoporosis, autoimmune thyroid disease, hypogonadism, and pituitary disorders.
-
Citations
Citations to this article as recorded by  - COVID-19 mRNA vaccine may trigger subacute thyroiditis
Mehmet Sözen, Ömercan Topaloğlu, Berrin Çetinarslan, Alev Selek, Zeynep Cantürk, Emre Gezer, Damla Köksalan, Taner Bayraktaroğlu
Human Vaccines & Immunotherapeutics.2024; 17(12): 5120. CrossRef - The role of co-morbidities in the development of an AEFI after COVID-19 vaccination in a large prospective cohort with patient-reported outcomes in the Netherlands
C. Ouaddouh, J.W. Duijster, T. Lieber, F.P.A.M. van Hunsel
Expert Opinion on Drug Safety.2024; 23(3): 323. CrossRef - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Prior immunization status of COVID-19 patients and disease severity: A multicenter retrospective cohort study assessing the different types of immunity
Javaria Aslam, Faisal Shahzad Khan, Muhammad Talha Haris, Hewad Hewadmal, Maryam Khalid, Mohammad Y. Alshahrani, Qurrat-ul-ain Aslam, Irrum Aneela, Urooj Zafar
Vaccine.2023; 41(2): 598. CrossRef - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(2): 253. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Inactivated SARS-CoV-2 vaccination does not disturb the clinical course of Graves’ disease: An observational cohort study
Shichen Xu, Huixin Yu, Xian Cheng, Jing Wu, Jiandong Bao, Li Zhang
Vaccine.2023; 41(38): 5648. CrossRef - Adrenal Crisis Associated With COVID-19 Vaccination in Patients With Adrenal Insufficiency
Yukako Kurematsu, Takako Mohri, Sadanori Okada, Yutaka Takahashi
JCEM Case Reports.2023;[Epub] CrossRef - Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Neue Aspekte der Glukokortikoidsubstitution bei Nebennierenrindeninsuffizienz
Tina Kienitz, Gesine Meyer
Der Internist.2022; 63(1): 12. CrossRef - Endocrine Follow-up During Post-Acute COVID-19: Practical Recommendations Based on Available Clinical Evidence
Rimesh Pal, Ameya Joshi, Sanjay K. Bhadada, Mainak Banerjee, Suresh Vaikkakara, Satinath Mukhopadhyay
Endocrine Practice.2022; 28(4): 425. CrossRef - Safety of Inactivated and mRNA COVID-19 Vaccination Among Patients Treated for Hypothyroidism: A Population-Based Cohort Study
Xi Xiong, Carlos King Ho Wong, Ivan Chi Ho Au, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Kristy Tsz Kwan Lau, Chi Ho Lee, Yu Cho Woo, David Tak Wai Lui, Ian Chi Kei Wong
Thyroid.2022; 32(5): 505. CrossRef - The New Entity of Subacute Thyroiditis amid the COVID-19 Pandemic: From Infection to Vaccine
Mihaela Popescu, Adina Ghemigian, Corina Maria Vasile, Andrei Costache, Mara Carsote, Alice Elena Ghenea
Diagnostics.2022; 12(4): 960. CrossRef - Adrenal Crisis Secondary to COVID-19 Vaccination in a Patient With Hypopituitarism
Nikolina Markovic, Anila Faizan, Chirag Boradia, Sridhar Nambi
AACE Clinical Case Reports.2022; 8(4): 171. CrossRef - The Effect of Inactivated SARS-CoV-2 Vaccines on TRAB in Graves’ Disease
LingHong Huang, ZhengRong Jiang, JingXiong Zhou, YuPing Chen, HuiBin Huang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Osteoporosis in Patients With Respiratory Diseases
Yue Ma, Shui Qiu, Renyi Zhou
Frontiers in Physiology.2022;[Epub] CrossRef - Pilot Findings on SARS-CoV-2 Vaccine-Induced Pituitary Diseases: A Mini Review from Diagnosis to Pathophysiology
Ach Taieb, El Euch Mounira
Vaccines.2022; 10(12): 2004. CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - No need of glucocorticoid dose adjustment in patients with adrenal insufficiency before COVID-19 vaccine
Tania Pilli, Cristina Dalmiglio, Gilda Dalmazio, Alfonso Sagnella, Raffaella Forleo, Lucia Brilli, Fabio Maino, Cristina Ciuoli, Maria Grazia Castagna
European Journal of Endocrinology.2022; 187(1): K7. CrossRef - Diabetes and COVID-19 Vaccination
Hae Dong Choi, Jun Sung Moon
The Journal of Korean Diabetes.2021; 22(4): 221. CrossRef
- Clinical Study
- Development and Validation of a Risk Scoring System Derived from Meta-Analyses of Papillary Thyroid Cancer
-
Sunghwan Suh, Tae Sik Goh, Yun Hak Kim, Sae-Ock Oh, Kyoungjune Pak, Ju Won Seok, In Joo Kim
-
Endocrinol Metab. 2020;35(2):435-442. Published online June 24, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.2.435
-
Correction in: Endocrinol Metab 2023;38(2):287
-
5,600
View
-
130
Download
-
3
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The aim of this study was to develop a scoring system to stratify the risk of papillary thyroid cancer (PTC) and to select the proper management.
Methods
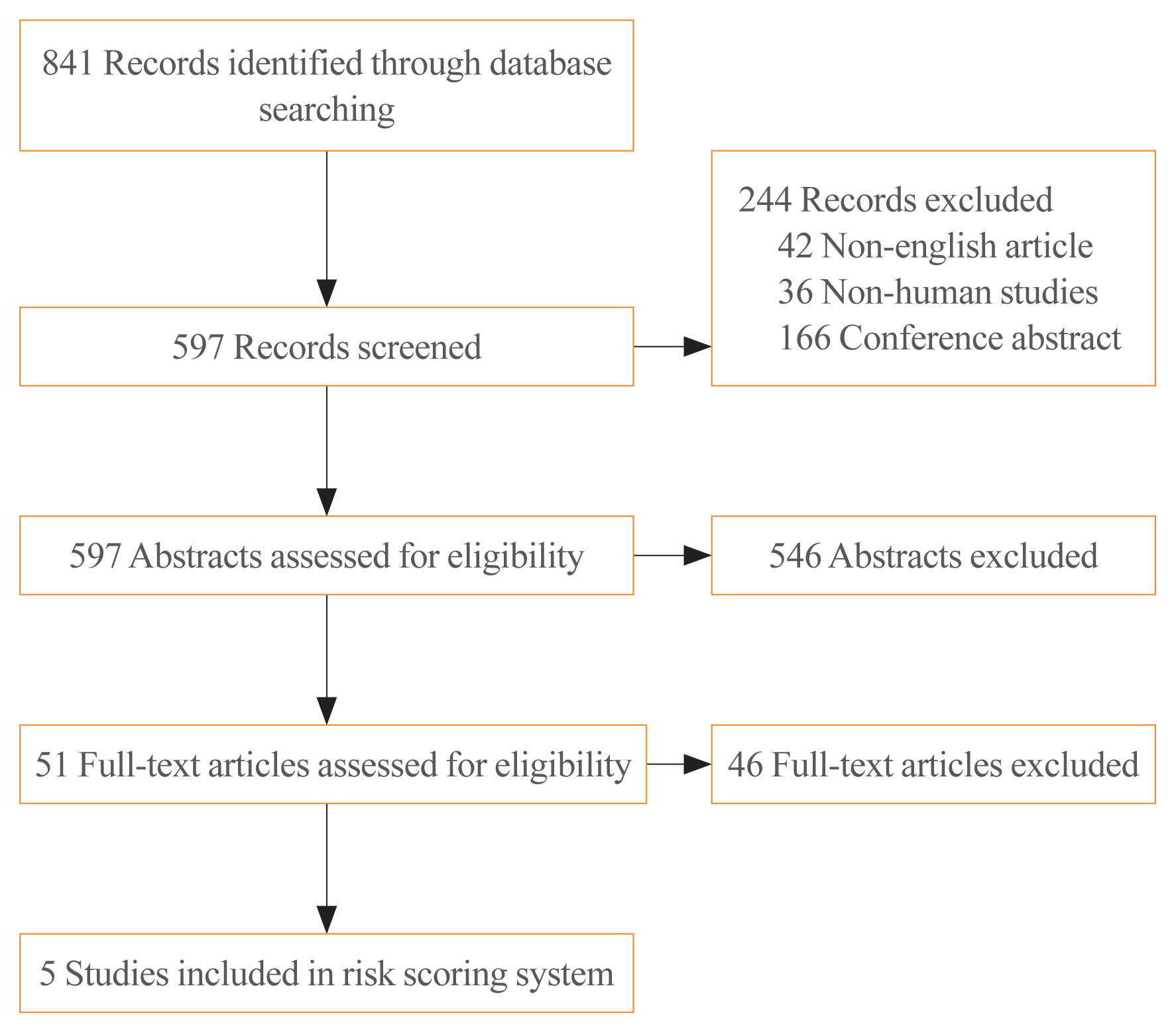
We performed a systematic search of MEDLINE and Embase. Data regarding patients’ prognoses were obtained from the included studies. Odds ratios (ORs) with statistical significance were extracted from the publications. To generate a risk scoring system (RSS), ORs were summed (RSS1), and summed after natural-logarithmic transformation (RSS2). RSS1 and RSS2 were compared to the eighth edition of the American Joint Committee on Cancer (AJCC) staging system and the 2015 American Thyroid Association (ATA) guidelines for thyroid nodules and differentiated thyroid carcinoma.
Results
Five meta-analyses were eligible for inclusion in the study. Eight variables (sex, tumour size, extrathyroidal extension, BRAF mutation, TERT mutation, histologic subtype, lymph node metastasis, and distant metastasis) were included. RSS1 was the best of the analysed models.
Conclusion
We developed and validated a new RSS derived from previous meta-analyses for patients with PTC. This RSS seems to be superior to previously published systems.
-
Citations
Citations to this article as recorded by  - Investigating 18F-FDG PET/CT Parameters as Prognostic Markers for Differentiated Thyroid Cancer: A Systematic Review
Hongxi Wang, Hongyuan Dai, Qianrui Li, Guohua Shen, Lei Shi, Rong Tian
Frontiers in Oncology.2021;[Epub] CrossRef - Impact of Multifocality on the Recurrence of Papillary Thyroid Carcinoma
Joohyun Woo, Hyeonkyeong Kim, Hyungju Kwon
Journal of Clinical Medicine.2021; 10(21): 5144. CrossRef
- Glucocorticoid-Induced Diabetes Mellitus: An Important but Overlooked Problem
-
Sunghwan Suh, Mi Kyoung Park
-
Endocrinol Metab. 2017;32(2):180-189. Published online May 29, 2017
-
DOI: https://doi.org/10.3803/EnM.2017.32.2.180
-
-
15,389
View
-
595
Download
-
108
Web of Science
-
117
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
Glucocorticoids are widely used as potent anti-inflammatory and immunosuppressive drugs to treat a wide range of diseases. However, they are also associated with a number of side effects, including new-onset hyperglycemia in patients without a history of diabetes mellitus (DM) or severely uncontrolled hyperglycemia in patients with known DM. Glucocorticoid-induced diabetes mellitus (GIDM) is a common and potentially harmful problem in clinical practice, affecting almost all medical specialties, but is often difficult to detect in clinical settings. However, scientific evidence is lacking regarding the effects of GIDM, as well as strategies for prevention and treatment. Similarly to nonsteroid-related DM, the principles of early detection and risk factor modification apply. Screening for GIDM should be considered in all patients treated with medium to high doses of glucocorticoids. Challenges in the management of GIDM stem from wide fluctuations in postprandial hyperglycemia and the lack of clearly defined treatment protocols. Together with lifestyle measures, hypoglycemic drugs with insulin-sensitizing effects are indicated. However, insulin therapy is often unavoidable, to the point that insulin can be considered the drug of choice. The treatment of GIDM should take into account the degree and pattern of hyperglycemia, as well as the type, dose, and schedule of glucocorticoid used. Moreover, it is essential to instruct the patient and/or the patient's family about how to perform the necessary adjustments. Prospective studies are needed to answer the remaining questions regarding GIDM. -
Citations
Citations to this article as recorded by 
- Clinical Study
- Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
-
Sunghwan Suh, Mi Yeon Kim, Soo Kyoung Kim, Kyu Yeon Hur, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
-
Endocrinol Metab. 2016;31(1):134-141. Published online March 16, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.1.134
-
-
3,839
View
-
44
Download
-
7
Web of Science
-
6
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Incretin hormone levels as a predictor of type 2 diabetes mellitus have not been fully investigated. Therefore, we measured incretin hormone levels to examine the relationship between circulating incretin hormones, diabetes, and future diabetes development in this study. MethodsA nested case-control study was conducted in a Korean cohort. The study included the following two groups: the control group (n=149), the incident diabetes group (n=65). Fasting total glucagon-like peptide-1 (GLP-1) and total glucose-dependent insulinotropic peptide (GIP) levels were measured and compared between these groups. ResultsFasting total GIP levels were higher in the incident diabetes group than in the control group (32.64±22.68 pmol/L vs. 25.54±18.37 pmol/L, P=0.034). There was no statistically significant difference in fasting total GLP-1 levels between groups (1.14±1.43 pmol/L vs. 1.39±2.13 pmol/L, P=0.199). In multivariate analysis, fasting total GIP levels were associated with an increased risk of diabetes (odds ratio, 1.005; P=0.012) independent of other risk factors. ConclusionFasting total GIP levels may be a risk factor for the development of type 2 diabetes mellitus. This association persisted even after adjusting for other metabolic parameters such as elevated fasting glucose, hemoglobin A1c, and obesity in the pre-diabetic period.
-
Citations
Citations to this article as recorded by  - Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes
Karlijn A. C. Meeks, Amy R. Bentley, Themistocles L. Assimes, Nora Franceschini, Adebowale A. Adeyemo, Charles N. Rotimi, Ayo P. Doumatey
Genome Medicine.2023;[Epub] CrossRef - Glucose- and Bile Acid-Stimulated Secretion of Gut Hormones in the Isolated Perfused Intestine Is Not Impaired in Diet-Induced Obese Mice
Jenna E. Hunt, Jens J. Holst, Sara L. Jepsen
Frontiers in Endocrinology.2022;[Epub] CrossRef - Combined treatment with a gastric inhibitory polypeptide receptor antagonist and a peptidyl peptidase-4 inhibitor improves metabolic abnormalities in diabetic mice
Fei Yang, Shan Dang, Hongjun LV, Bingyin Shi
Journal of International Medical Research.2021; 49(1): 030006052098566. CrossRef - Elevated levels of fasting serum GIP may be protective factors for diabetic retinopathy in type 2 diabetes mellitus
LingHong Huang, JingXiong Zhou, Bo Liang, HuiBin Huang, LiangYi Li
International Journal of Diabetes in Developing Countries.2021; 41(4): 543. CrossRef - Enteroendocrine K and L cells in healthy and type 2 diabetic individuals
Tina Jorsal, Nicolai A. Rhee, Jens Pedersen, Camilla D. Wahlgren, Brynjulf Mortensen, Sara L. Jepsen, Jacob Jelsing, Louise S. Dalbøge, Peter Vilmann, Hazem Hassan, Jakob W. Hendel, Steen S. Poulsen, Jens J. Holst, Tina Vilsbøll, Filip K. Knop
Diabetologia.2018; 61(2): 284. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Thyroid
- Subclinical Hypothyroidism and Cardiovascular Disease
-
Sunghwan Suh, Duk Kyu Kim
-
Endocrinol Metab. 2015;30(3):246-251. Published online August 4, 2015
-
DOI: https://doi.org/10.3803/EnM.2015.30.3.246
-
-
4,967
View
-
68
Download
-
31
Web of Science
-
29
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
Subclinical hypothyroidism (SCH) is a common disorder that is characterized by elevated thyroid-stimulating hormone levels in conjunction with free thyroxine concentrations within the normal reference range. Thyroid hormones are known to affect the heart and vasculature and, as a result, the impact of SCH on the cardiovascular (CV) system has recently become an important topic of research. Strong evidence points to a link between SCH and CV risk factors such as alterations in blood pressure, lipid levels, and atherosclerosis. Additionally, accumulating evidence indicates that SCH is associated with metabolic syndrome and heart failure. The present review proposes that SCH may be a potentially modifiable risk factor of CV disease and mortality. However, large-scale clinical trials with appropriate power investigating the risks and benefits of SCH treatment are required to determine whether these benefits can be achieved with levothyroxine therapy. -
Citations
Citations to this article as recorded by  - Prognostic implications of thyroid disease in patients with atrial fibrillation
Anthi Vasilopoulou, Vasiliki Patsiou, Alexandra Bekiaridou, Andreas S. Papazoglou, Dimitrios V. Moysidis, Marina Spaho, Martha Zergioti, Dimitrios Kostakakis, Maria-Eirini Kyriakideli, Chrysanthi-Ioanna Lampropoulou, Anastasios Kartas, Athanasios Samaras,
Heart and Vessels.2024; 39(2): 185. CrossRef - A Comparative Study of Iron Status in Subclinical Hypothyroid and Euthyroid Subjects in a Tertiary Care Hospital
Thokati G Swapnika, S S Sabitha Rani, Satish Dipankar, Afreen Begum H Itagi, Immadi S Vamshidhar
Cureus.2024;[Epub] CrossRef - The influence of hypothyroidism on the course of coronary artery disease in patients with reduced left ventricular ejection fraction
M.V. Kucheriava, G.B. Mankovskyi
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2023; 19(3): 161. CrossRef - Correlation between Subclinical Hypothyroidism and Metabolic Syndrome: A Retrospective Study
SalhahSaleh Alsulami, Mukhtiar Baig, AtheerHameed Albeladi, ShahadBandar Alyoubi, ShahadAlhumaidi Alsubaie, SamahAbdulsalam Albeladi, KholoudAlawi Ghamri, AbeerMohammed Saeed Alraiqi, SafaMobarak Alyoubi, WesamAied Almutairi
Saudi Journal of Medicine and Medical Sciences.2023; 11(3): 250. CrossRef - Low awareness and under-diagnosis of hypothyroidism
Ulrike Gottwald-Hostalek, Barbara Schulte
Current Medical Research and Opinion.2022; 38(1): 59. CrossRef - Mean platelet volume (MPV) levels in subclinical hypothyroidism and its relation to serum lipid levels
Zafer ERCAN, Mehmet Emin DEMİR
Anatolian Current Medical Journal.2022; 4(3): 234. CrossRef - The impact of subclinical hypothyroidism on long-term outcomes in older patients undergoing percutaneous coronary intervention
Yong-Sheng Liu, Mei Wei, Le Wang, Gang Liu, Guo-Ping Ma, Katsushige Ono, Ze-Long Cao, Man Yang, Ming-Qi Zheng
BMC Endocrine Disorders.2021;[Epub] CrossRef - Subclinical Hypothyroidism in Geriatric Population and Its Association With Heart Failure
Priyanka Panday, Ana P Arcia Franchini, Beshoy Iskander, Fatima Anwer, Federico Oliveri, Fotios Kakargias , Pousette Hamid
Cureus.2021;[Epub] CrossRef - The Effect of Thyroxine Therapy on Cardiovascular Risk Factors in Patients with Subclinical Hypothyroidism
Selvihan BEYSEL, Mahmut APAYDIN, Mustafa ÇALIŞKAN, Mustafa ÖZBEK, Erman ÇAKAL
Düzce Üniversitesi Sağlık Bilimleri Enstitüsü Dergisi.2021;[Epub] CrossRef - Pathophysiological aspects of development myocardial infarction type 2 in subclinical hypothyroidism
A. A. Ivannikov, A. A. Kanibolotsky, Kh. G. Alidzhanova, I. V. Bratischev
Medical alphabet.2021; (42): 34. CrossRef - Unknown Subclinical Hypothyroidism and In-Hospital Outcomes and Short- and Long-Term All-Cause Mortality among ST Segment Elevation Myocardial Infarction Patients Undergoing Percutaneous Coronary Intervention
Elena Izkhakov, David Zahler, Keren-Lee Rozenfeld, Dor Ravid, Shmuel Banai, Yan Topilsky, Naftali Stern, Yona Greenman, Yacov Shacham
Journal of Clinical Medicine.2020; 9(12): 3829. CrossRef - Evaluation of left atrial volume and functions by real time three‐dimensional echocardiography in patients with subclinical hypothyroidism before and after levothyroxine therapy
Seçkin Dereli, Adil Bayramoğlu, Nurtaç Özer, Ahmet Kaya, Muhammet Özbilen
Echocardiography.2019; 36(5): 916. CrossRef - The impact of thyroid hormone dysfunction on ischemic heart disease
Madalena von Hafe, João Sergio Neves, Catarina Vale, Marta Borges-Canha, Adelino Leite-Moreira
Endocrine Connections.2019; 8(5): R76. CrossRef - Association High-Iodine-Containing Seaweed Soup Consumption after Birth and Subclinical Hypothyroidism in Korean Women: Korea National Health and Nutrition Examination Survey IV (2013–2015)
Hyunsam Kim, Ha Ni Lee, Jeonghoon Ha
International Journal of Thyroidology.2019; 12(2): 105. CrossRef - Association between subclinical hypothyroidism and metabolic disorders: A retrospective chart review study in an emerging university hospital
Khaled Aldossari, Sameer Al‐Ghamdi, Jamaan Al‐Zahrani, Anwar Al Jammah, Bader Alanazi, Abdulilah Al‐Briek, Mohammad Alanazi
Journal of Clinical Laboratory Analysis.2019;[Epub] CrossRef - Thyroid replacement therapy, thyroid stimulating hormone concentrations, and long term health outcomes in patients with hypothyroidism: longitudinal study
Rasiah Thayakaran, Nicola J Adderley, Christopher Sainsbury, Barbara Torlinska, Kristien Boelaert, Dana Šumilo, Malcolm Price, G Neil Thomas, Konstantinos A Toulis, Krishnarajah Nirantharakumar
BMJ.2019; : l4892. CrossRef - Visceral Adiposity Index Levels in Patients with Hypothyroidism
Selma Pekgor, Cevdet Duran, Ruhuşen Kutlu, Ibrahim Solak, Ahmet Pekgor, Mehmet Ali Eryilmaz
Journal of the National Medical Association.2018; 110(6): 606. CrossRef - Diagnosis and Management of Hypothyroidism: Addressing the Knowledge–Action Gaps
Sanjay Kalra, A. K. Das, Sarita Bajaj, Banshi Saboo, Deepak Khandelwal, Mangesh Tiwaskar, Navneet Agarwal, Pritam Gupta, Rakesh Sahay, Sameer Aggarwal, Sujoy Ghosh, Vijay Negalur, A. G. Unnikrishnan, Ganapathi Bantwal, Rashmi Aggarwal, Harshal Chaudhari,
Advances in Therapy.2018; 35(10): 1519. CrossRef - DYNAMICS OF EXCHANGE PARAMETERS OF ULTRASONIC HEART RESEARCH IN PATIENTS WITH CLIMACTERIC SYNDROME ASSOCIATED WITH HYPOTHYROIDISM UNDER THE INFLUENCE OF COMPLEX THERAPY
M. O. Pavlovska, V. P. Vakaluk, E. I. Deltsova
World of Medicine and Biology.2018; 14(63): 056. CrossRef - Risk factors for cardiovascular disease in subclinical hypothyroidism
F. Decandia
Irish Journal of Medical Science (1971 -).2018; 187(1): 39. CrossRef - New levothyroxine formulation meeting 95–105% specification over the whole shelf-life: results from two pharmacokinetic trials
Ulrike Gottwald-Hostalek, Wolfgang Uhl, Peter Wolna, George J. Kahaly
Current Medical Research and Opinion.2017; 33(2): 169. CrossRef - Subclinical thyroid dysfunction and risk of carotid atherosclerosis
Hosu Kim, Tae Hyuk Kim, Hye In Kim, So Young Park, Young Nam Kim, Seonwoo Kim, Min-Ji Kim, Sang-Man Jin, Kyu Yeon Hur, Jae Hyeon Kim, Moon-Kyu Lee, Yong-Ki Min, Jae Hoon Chung, Mira Kang, Sun Wook Kim, Tatsuo Shimosawa
PLOS ONE.2017; 12(7): e0182090. CrossRef - Effect of Marijuana Use on Thyroid Function and Autoimmunity
Sonali Malhotra, Rubina A. Heptulla, Peter Homel, Roja Motaghedi
Thyroid.2017; 27(2): 167. CrossRef - Modified Low-Dose Triiodo-L-thyronine Therapy Safely Improves Function Following Myocardial Ischemia-Reperfusion Injury
Viswanathan Rajagopalan, Youhua Zhang, Christine Pol, Clifford Costello, Samantha Seitter, Ann Lehto, Olga V. Savinova, Yue-feng Chen, A. Martin Gerdes
Frontiers in Physiology.2017;[Epub] CrossRef - Myocardial Performance Index for Patients with Overt and Subclinical Hypothyroidism
Aziz Karabulut, Abdullah Doğan, Alpaslan Kemal Tuzcu
Medical Science Monitor.2017; 23: 2519. CrossRef - CARDIOVASCULAR MANIFESTATIONS IN PATIENTS OF HYPOTHYROIDISM- RESULTS OF A SINGLE CENTRE STUDY
Rohit Vasant Deshpande, Swati Harish Sharma, Swapnil Sahebrao Walke, Mayur Ramakrishnarao Hedau, Bharat Sing Rathod, Amol Raghunath Bhore, Hitesh Lotan Mahale
Journal of Evolution of Medical and Dental Sciences.2017; 6(45): 3514. CrossRef - The Association of Thyroid Hormones and Tsh with the Metabolic Syndrome in Euthyroid Taiwanese Individuals
Chun-Yuan Huang, Lee-Ching Hwang
Endocrine Practice.2016; 22(11): 1303. CrossRef - Potential harmful correlation between homocysteine and low-density lipoprotein cholesterol in patients with hypothyroidism
Xuejie Dong, Zhi Yao, Yanjin Hu, Ning Yang, Xia Gao, Yuan Xu, Guang Wang
Medicine.2016; 95(29): e4291. CrossRef - Impaired Hemorheological Parameters and Increased Carotid Intima-Media Thickness in Children with Subclinical Hypothyroidism
Yasemin Isik-Balci, Sebahat Agladioglu, Kadir Agladioglu, Emine Kilic-Toprak, Ozgen Kilic-Erkek, Bayram Ozhan, Aziz Polat, Melek Bor-Kucukatay
Hormone Research in Paediatrics.2016; 85(4): 250. CrossRef
- Obesity and Metabolism
- Metformin-Associated Lactic Acidosis
-
Sunghwan Suh
-
Endocrinol Metab. 2015;30(1):45-46. Published online March 27, 2015
-
DOI: https://doi.org/10.3803/EnM.2015.30.1.45
-
-
3,392
View
-
43
Download
-
5
Web of Science
-
5
Crossref
-
 PDF PDF PubReader PubReader
-
Citations
Citations to this article as recorded by  - Compuestos bioactivos de canela y su efecto en la disminución del síndrome metabólico: revisión sistemática
Fernanda Riós, Aurora Quintero, Javier Piloni, Raquel Cariño, Abigail Reyes
Archivos Latinoamericanos de Nutrición.2023; 73(1): 74. CrossRef - Impacts of metformin on tuberculosis incidence and clinical outcomes in patients with diabetes: a systematic review and meta-analysis
Meng Zhang, Jian-qing He
European Journal of Clinical Pharmacology.2020; 76(2): 149. CrossRef - Metformin: A review of its therapeutic efficacy and adverse effects
Noura T. Shurrab, El-Shaimaa A. Arafa
Obesity Medicine.2020; 17: 100186. CrossRef - Association between Metformin Use and Risk of Lactic Acidosis or Elevated Lactate Concentration in Type 2 Diabetes
Eun Young Lee, Sena Hwang, Yong-ho Lee, Seo Hee Lee, Young Mi Lee, Hua Pyong Kang, Eugene Han, Woonhyoung Lee, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Yonsei Medical Journal.2017; 58(2): 312. CrossRef - Metformin associated lactic acidosis (MALA): clinical profiling and management
Alessandra Moioli, Barbara Maresca, Andrea Manzione, Antonello Maria Napoletano, Daniela Coclite, Nicola Pirozzi, Giorgio Punzo, Paolo Menè
Journal of Nephrology.2016; 29(6): 783. CrossRef
- Adrenal gland
- Clinical Characteristics, Management, and Outcome of 22 Cases of Primary Hypophysitis
-
Sun Mi Park, Ji Cheol Bae, Ji Young Joung, Yoon Young Cho, Tae Hun Kim, Sang-Man Jin, Sunghwan Suh, Kyu Yeon Hur, Kwang-Won Kim
-
Endocrinol Metab. 2014;29(4):470-478. Published online December 29, 2014
-
DOI: https://doi.org/10.3803/EnM.2014.29.4.470
-
-
4,275
View
-
41
Download
-
26
Web of Science
-
24
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Primary hypophysitis causes varying degrees of endocrine dysfunction and mass effect. The natural course and best treatment have not been well established. MethodsMedical records of 22 patients who had been diagnosed with primary hypophysitis between January 2001 and March 2013 were retrospectively reviewed. Based on the anatomical location, we classified the cases as adenohypophysitis (AH), infundibuloneurohypophysitis (INH), and panhypophysitis (PH). Clinical presentation, endocrine function, pathologic findings, magnetic resonance imaging findings, and treatment courses were reviewed. ResultsAmong 22 patients with primary hypophysitis, 81.8% (18/22) had involvement of the posterior pituitary lobe. Two patients of the AH (2/3, 66.6%) and three patients of the PH (3/10, 30%) groups initially underwent surgical mass reduction. Five patients, including three of the PH (3/10, 33.3%) group and one from each of the AH (1/3, 33.3%) and INH (1/9, 11.1%) groups, initially received high-dose glucocorticoid treatment. Nearly all of the patients treated with surgery or high-dose steroid treatment (9/11, 82%) required continuous hormone replacement during the follow-up period. Twelve patients received no treatment for mass reduction due to the absence of acute symptoms and signs related to a compressive mass effect. Most of them (11/12, 92%) did not show disease progression, and three patients recovered partially from hormone deficiency. ConclusionDeficits of the posterior pituitary were the most common features in our cases of primary hypophysitis. Pituitary endocrine defects responded less favorably to glucocorticoid treatment and surgery. In the absence of symptoms related to mass effect and with the mild defect of endocrine function, it may not require treatment to reduce mass except hormone replacement.
-
Citations
Citations to this article as recorded by  - Secondary xanthogranulomatous hypophysitis mimicking a pituitary macroadenoma: a case report
Salma Salhi, Ibtissem Oueslati, Yasmine Mouelhi, Alia Zehani, Nidhameddine Kchir, Elyes Kamoun, Meriem Yazidi, Melika Chihaoui
Journal of International Medical Research.2024;[Epub] CrossRef - Glucocorticoid therapy as first-line treatment in primary hypophysitis: a systematic review and individual patient data meta-analysis
Brijesh Krishnappa, Ravikumar Shah, Saba Samad Memon, Chakra Diwaker, Anurag R Lila, Virendra A Patil, Nalini S Shah, Tushar R Bandgar
Endocrine Connections.2023;[Epub] CrossRef - Hypophysitis, the Growing Spectrum of a Rare Pituitary Disease
Fabienne Langlois, Elena V Varlamov, Maria Fleseriu
The Journal of Clinical Endocrinology & Metabolism.2022; 107(1): 10. CrossRef - Outcomes of Initial Management Strategies in Patients With Autoimmune Lymphocytic Hypophysitis: A Systematic Review and Meta-analysis
Diane Donegan, Zeb Saeed, Danae A Delivanis, Mohammad Hassan Murad, Juergen Honegger, Felix Amereller, Seda Hanife Oguz, Dana Erickson, Irina Bancos
The Journal of Clinical Endocrinology & Metabolism.2022; 107(4): 1170. CrossRef - Early Pulse Glucocorticoid Therapy and Improved Hormonal Outcomes in Primary Hypophysitis
Brijesh Krishnappa, Ravikumar Shah, Vijaya Sarathi, Anurag Ranjan Lila, Manjeet Kaur Sehemby, Virendra A. Patil, Shilpa Sankhe, Nalini Shah, Tushar Bandgar
Neuroendocrinology.2022; 112(2): 186. CrossRef - Preoperative differentiation of hypophysitis and pituitary adenomas using a novel clinicoradiologic scoring system
Kyla Wright, Hyon Kim, Travis Hill, Matthew Lee, Cordelia Orillac, Nikita Mogar, Donato Pacione, Nidhi Agrawal
Pituitary.2022; 25(4): 602. CrossRef - Hypophysitis
Diane Donegan, Jürgen Honegger
Endocrine Practice.2022; 28(9): 901. CrossRef - Rare Case of a Disappearing Pituitary Adenoma During the Coronavirus Disease 2019 (COVID-19) Pandemic
David P. Bray, C. Arturo Solares, Nelson M. Oyesiku
World Neurosurgery.2021; 146: 148. CrossRef - Diabetes insipidus secondary to sellar/parasellar lesions
Anna Angelousi, Chrysoula Mytareli, Paraskevi Xekouki, Eva Kassi, Konstantinos Barkas, Ashley Grossman, Gregory Kaltsas
Journal of Neuroendocrinology.2021;[Epub] CrossRef - Clinical presentation and management of hypophysitis: An observational study of case series
Marouan Karrou, Salma Benyakhlef, Achwak Alla, Najoua Messaoudi, Asmae Oulad Amar, Siham Rouf, Imane Kamaoui, Noureddine Oulali, Faycal Moufid, Naima Abda, Hanane Latrech
Surgical Neurology International.2021; 12: 304. CrossRef - Clinical aspects of autoimmune hypothalamitis, a variant of autoimmune hypophysitis: Experience from one center
Qian Wei, Guoqing Yang, Zhaohui Lue, Jingtao Dou, Li Zang, Yijun Li, Jin Du, Weijun Gu, Yiming Mu
Journal of International Medical Research.2020; 48(3): 030006051988783. CrossRef - Primary and Ipilimumab-induced Hypophysitis: A Single-center Case Series
Paul Atkins, Ehud Ur
Endocrine Research.2020; 45(4): 246. CrossRef - Hypophysitis (Including IgG4 and Immunotherapy)
Anna Angelousi, Krystallenia Alexandraki, Marina Tsoli, Gregory Kaltsas, Eva Kassi
Neuroendocrinology.2020; 110(9-10): 822. CrossRef - Hypophysitis in the era of immune checkpoint inhibitors and immunoglobulin G4-related disease
Leen Wehbeh, Sama Alreddawi, Roberto Salvatori
Expert Review of Endocrinology & Metabolism.2019; 14(3): 167. CrossRef - Immune check point inhibitors-induced hypophysitis: a retrospective analysis of the French Pharmacovigilance database
Julie Garon-Czmil, Nadine Petitpain, Franck Rouby, Marion Sassier, Samy Babai, Mélissa Yéléhé-Okouma, Georges Weryha, Marc Klein, Pierre Gillet
Scientific Reports.2019;[Epub] CrossRef - Clinical Features, Magnetic Resonance Imaging, and Treatment Experience of 20 Patients with Lymphocytic Hypophysitis in a Single Center
Qiang Zhu, Ke Qian, Guijun Jia, Gang Lv, Jisheng Wang, Liyong Zhong, Shuqing Yu
World Neurosurgery.2019; 127: e22. CrossRef - Idiopathic granulomatous hypophysitis presenting with galactorrhea, headache, and nausea in a woman: a case report and review of the literature
Guive Sharifi, Mohammad Reza Mohajeri-Tehrani, Behrouz Navabakhsh, Bagher Larijani, Touraj Valeh
Journal of Medical Case Reports.2019;[Epub] CrossRef - Paciente de 31 años con polidipsia
A.R. Benavides Aramburu, M. Seguí Díaz
Medicina de Familia. SEMERGEN.2018; 44(2): e77. CrossRef - Primary hypophysitis and other autoimmune disorders of the sellar and suprasellar regions
Sriram Gubbi, Fady Hannah-Shmouni, Constantine A. Stratakis, Christian A. Koch
Reviews in Endocrine and Metabolic Disorders.2018; 19(4): 335. CrossRef - Primary lymphocytic hypophysitis: Clinical characteristics and treatment of 50 cases in a single centre in China over 18 years
Shuchang Wang, Linjie Wang, Yong Yao, Feng Feng, Hongbo Yang, Zhiyong Liang, Kan Deng, Hui You, Jian Sun, Bing Xing, Zimeng Jin, Renzhi Wang, Hui Pan, Huijuan Zhu
Clinical Endocrinology.2017; 87(2): 177. CrossRef - Clinical presentation and outcome of children with central diabetes insipidus associated with a self‐limited or transient pituitary stalk thickening, diagnosed as infundibuloneurohypophysitis
J. Schaefers, M. Cools, K. De Waele, I. Gies, V. Beauloye, P. Lysy, I. Francois, D. Beckers, J. De Schepper
Clinical Endocrinology.2017; 87(2): 171. CrossRef - Intrachiasmatic abscess caused by IgG4-related hypophysitis
Georgios F. Hadjigeorgiou, Eva Løbner Lund, Lars Poulsgaard, Ulla Feldt-Rasmussen, Åse Krogh Rasmussen, Marianne Wegener, Kåre Fugleholm
Acta Neurochirurgica.2017; 159(11): 2229. CrossRef - Granulomatous and lymphocytic hypophysitis – are they immunologically distinct?
Shilpa Rao, Anita Mahadevan, Tanmoy Maiti, Manish Ranjan, Shivayogi Durgad Shwetha, Arimappamagan Arivazhagan, Jitender Saini
APMIS.2016; 124(12): 1072. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef
- Obesity and Metabolism
- Sex Factors in the Metabolic Syndrome as a Predictor of Cardiovascular Disease
-
Sunghwan Suh, Jongha Baek, Ji Cheol Bae, Kyoung-Nyoun Kim, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
-
Endocrinol Metab. 2014;29(4):522-529. Published online December 29, 2014
-
DOI: https://doi.org/10.3803/EnM.2014.29.4.522
-
-
4,717
View
-
37
Download
-
16
Web of Science
-
17
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Metabolic syndrome (MetS) is a condition characterized by a cluster of metabolic disorders and is associated with increased risk of cardiovascular disease (CVD). This study analyzed data from the Korean Health and Genome Study to examine the impact of MetS on CVD. MethodsA total of 8,898 subjects (4,241 males and 4,657 females), 40 to 69 years of age, were enrolled and evaluated for the development of new onset CVD from 2001 to 2012 (median 8.1 years of follow-up). ResultsThe prevalence of MetS at baseline was 22.0% (932/4,241) and 29.7% (1,383/4,657) in males and females, respectively. MetS was associated with increased risk of coronary heart disease (CHD; hazard ratio [HR], 1.818; 95% confidence interval [CI], 1.312 to 2.520 in males; HR, 1.789; 95% CI, 1.332 to 2.404 in females) and CVD (HR, 1.689; 95% CI, 1.295 to 2.204 in males; HR, 1.686; 95% CI, 1.007 to 2.192 in females). Specifically, MetS was associated with risk of future stroke in females only (HR, 1.486; 95% CI, 1.007 to 2.192). Among MetS components, abdominal obesity and hypertension were independent predictors of both CHD and CVD. In addition, a higher number of MetS components correlated with higher CVD risk. ConclusionMetS is a significant risk factor for the development of CVD although its impact varies between sexes.
-
Citations
Citations to this article as recorded by  - Cardiovascular age of workers with different employment categories
Byung-Kook Lee, Jaeouk Ahn, Nam-Soo Kim, Jungsun Park, Yangho Kim
Archives of Environmental & Occupational Health.2022; 77(3): 243. CrossRef - Effects of Anthocyanin-rich Berries on the Risk of Metabolic Syndrome: A Systematic Review and Meta-analysis
Mikkel Roulund Wilken, Max Norman Tandrup Lambert, Christine Bodelund Christensen, Per Bendix Jeppesen
Review of Diabetic Studies.2022; 18(1): 42. CrossRef - Rate and risk factors of metabolic components and component combinations according to hypertension status in Tibetans in a cross-sectional study
Jihong Hu, Brian Thompson, Shuxia Wang, Minhao Guo, Chunjuan Yan, Fengfeng Ding, Peng Guo, Li Chen, Zhuoma Cao, Jianzong Wang
Medicine.2022; 101(43): e31320. CrossRef - Gender differences in changes in metabolic syndrome status and its components and risk of cardiovascular disease: a longitudinal cohort study
Azra Ramezankhani, Fereidoun Azizi, Farzad Hadaegh
Cardiovascular Diabetology.2022;[Epub] CrossRef - The Association of Metabolic Syndrome with the development of cardiovascular disease among Kazakhs in remote rural areas of Xinjiang, China: a cohort study
Wenwen Yang, Shuxia Guo, Haixia Wang, Yu Li, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Yanpeng Song, Changjing Li, Zhuo Ma, Rulin Ma, Jia He
BMC Public Health.2021;[Epub] CrossRef - Serum Arylsulfatase and Acid Phosphatase Activity in Patients with Metabolic Syndrome as a Result of Oxidative Damage to Lysosomes
Dorota M. Olszewska-Słonina
Protein & Peptide Letters.2021; 28(11): 1246. CrossRef - Validation of Risk Prediction Models for Atherosclerotic Cardiovascular Disease in a Prospective Korean Community-Based Cohort
Jae Hyun Bae, Min Kyong Moon, Sohee Oh, Bo Kyung Koo, Nam Han Cho, Moon-Kyu Lee
Diabetes & Metabolism Journal.2020; 44(3): 458. CrossRef - The Prevalence of Obesity and Metabolic Syndrome in the Korean Military Compared with the General Population
Jung Hwan Lee, Da Hea Seo, Min Jung Nam, Geon Hui Lee, Dong Hee Yang, Min Joo Lee, Ung-Rim Choi, Seongbin Hong
Journal of Korean Medical Science.2018;[Epub] CrossRef - Relationship between serum bilirubin levels and cardiovascular disease
Sunghwan Suh, Young Rak Cho, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee, Christian Herder
PLOS ONE.2018; 13(2): e0193041. CrossRef - Comparison Between Metabolic Syndrome and the Framingham Risk Score as Predictors of Cardiovascular Diseases Among Kazakhs in Xinjiang
Wenwen Yang, Rulin Ma, Xianghui Zhang, Heng Guo, Jia He, Lei Mao, Lati Mu, Yunhua Hu, Yizhong Yan, Jiaming Liu, Jiaolong Ma, Shugang Li, Yusong Ding, Mei Zhang, Jingyu Zhang, Shuxia Guo
Scientific Reports.2018;[Epub] CrossRef - Impact of interactions among metabolic syndrome components on the development of cardiovascular disease among Kazakhs in Xinjiang
Wenwen Yang, Xiang Gao, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jia He, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Shugang Li, Yusong Ding, Mei Zhang, Rulin Ma, Shuxia Guo, Mahesh Narayan
PLOS ONE.2018; 13(10): e0205703. CrossRef - Prediction of cardiovascular disease in Korean population: based on health risk appraisal of national health screening program
Jae Moon Yun, Tae Gon Yoo, Seung-Won Oh, Be Long Cho, Eunyoung Kim, Insob Hwang
Journal of the Korean Medical Association.2017; 60(9): 746. CrossRef - Metabolic Syndrome Is a Strong Risk Factor for Minor Ischemic Stroke and Subsequent Vascular Events
Guang-Sheng Wang, Dao-Ming Tong, Xiao-Dong Chen, Tong-Hui Yang, Ye-Ting Zhou, Xiao-Bo Ma, Gianpaolo Reboldi
PLOS ONE.2016; 11(8): e0156243. CrossRef - Metabolic syndrome related to cardiovascular events in a 10-year prospective study
Laura Kazlauskienė, Jūratė Butnorienė, Antanas Norkus
Diabetology & Metabolic Syndrome.2015;[Epub] CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Impact of Cadmium Exposure on the Association between Lipopolysaccharide and Metabolic Syndrome
Seung Han, Kyoung Ha, Ja Jeon, Hae Kim, Kwan Lee, Dae Kim
International Journal of Environmental Research and Public Health.2015; 12(9): 11396. CrossRef - Heat Killed Lactobacillus reuteri GMNL-263 Reduces Fibrosis Effects on the Liver and Heart in High Fat Diet-Hamsters via TGF-β Suppression
Wei-Jen Ting, Wei-Wen Kuo, Dennis Hsieh, Yu-Lan Yeh, Cecilia-Hsuan Day, Ya-Hui Chen, Ray-Jade Chen, Viswanadha Padma, Yi-Hsing Chen, Chih-Yang Huang
International Journal of Molecular Sciences.2015; 16(10): 25881. CrossRef
|